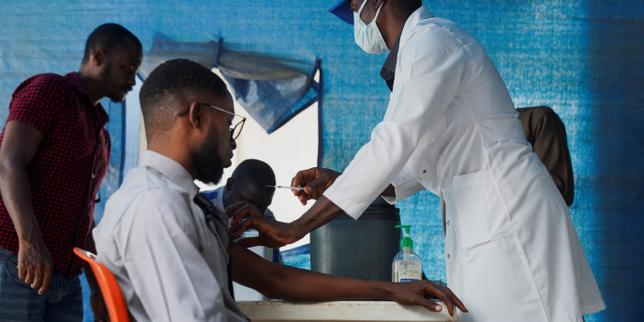
Somalia's health system isn't just "under pressure" anymore. It's effectively being dismantled by a checkbook. While the world's attention drifts toward newer headlines, a quiet, mathematical catastrophe is unfolding across the Horn of Africa. We're seeing a 67% collapse in international humanitarian funding this year, and the math of that deficit is written in closed clinic doors and empty medicine cabinets.
I've looked at the numbers, and they're grim. By mid-2026, experts expect a 35% reduction in the number of functioning health facilities across the country. We aren't talking about losing "extra" services. We're talking about losing the bare essentials: vaccinations, clean births, and the therapeutic peanut paste that keeps a malnourished child's heart beating.
The Brutal Reality of the Funding Gap
Most people don't realize how much Somalia relies on the outside world just to keep the lights on in a local ward. About 95% of the country's health budget comes from external financing. When those donors pull back—whether because of "aid fatigue" or shifting geopolitical priorities—the system doesn't just lean; it breaks.
Right now, more than 200 health facilities have already shut down. Another 300 are on the literal brink of following suit in the next few months. If you're a mother in a rural district, your "local" clinic might have just vanished, replaced by a twelve-hour walk you can't afford to take.
Why the Money is Vanishing
It's a perfect storm of bad timing. Global inflation has made everything from fuel to bandages more expensive. At the same time, major donor nations are tightening their belts or redirecting funds to conflicts in Europe and the Middle East.
- Humanitarian Response Plan (HNRP): In 2025, the plan was only 27% funded.
- UNICEF’s Appeal: Their health and nutrition efforts faced an 82% funding gap by the end of last year.
- The Result: 6.5 million people are now facing crisis-level hunger, and there’s no safety net to catch them when they fall ill from it.
The Malnutrition Loop
You can't separate hunger from health. When a child doesn't eat, their immune system shuts down. In Somalia, we're seeing a 79% rise in moderate acute malnutrition cases at some clinics. These kids aren't just hungry; they're vulnerable to everything from measles to cholera.
It's a vicious cycle. A drought kills the livestock, the family loses their income, the children stop eating, they get sick with a preventable disease, and then they find out the local clinic has closed because the funding for the staff's salaries dried up three months ago. Honestly, it’s a miracle the system has held on this long.
The Cost of a Hospital Visit
For those lucky enough to find a clinic that's still open, the price of getting there is the next hurdle. Fuel prices in Somalia have spiked due to global supply shocks. For a family in Baidoa or Mudug, the cost of a truck ride to the city can be more than a month's worth of food.
I’ve seen reports of parents walking for half a day with a sick infant because they couldn't scrape together the cash for transport. By the time they arrive, the child is often in critical condition. When we cut aid, we aren't just "saving money"—we're shifting a massive financial and physical burden onto the people who have the least.
Transitioning from Aid to Ownership
The Federal Government of Somalia knows it can't live on handouts forever. They've launched the Centennial Vision 2060, a plan to turn the country into a middle-income nation over the next few decades. It's an ambitious roadmap that focuses on building a "capable state" that can actually serve its people.
But here’s the problem: you can't build a 2060 economy on the backs of a generation that’s currently dying of measles.
- Domestic Revenue: The government is trying to increase tax collection to fund its own services, but the share of the national budget going to health is still under 7%.
- Parallel Systems: For years, aid went around the government rather than through it. This created "vertical" programs—one for polio, one for malaria—that didn't help build a unified national hospital system.
- The Goal: Moving toward Universal Health Coverage (UHC) where the Somali Ministry of Health, not an NGO in London or Geneva, calls the shots.
What Needs to Happen Now
We need to stop treating Somalia like a series of one-off emergencies and start treating it like a long-term investment. If the funding doesn't stabilize, we're going to see a total reversal of the public health gains made over the last decade.
- Flexible Funding: Donors need to move away from "earmarked" money that can only be used for one specific disease. The system needs "flexible" cash to keep clinics open and staff paid.
- Infrastructure Support: Instead of just sending medicine, we need to invest in the boreholes and solar power that keep hospitals functional during climate shocks.
- Local Integration: Aid agencies must stop running parallel systems and start folding their staff and data into the Somali National Health Sector Strategic Plan.
The situation is dire, but it's not hopeless. It’s a choice. We can either pay the price now to keep these clinics open, or we can pay a much higher price later when a massive, preventable health crisis spills across borders. The breaking point isn't coming; for many Somali families, it's already here.
You can support organizations like Médecins Sans Frontières (MSF) or the International Rescue Committee (IRC) that are still on the ground, but the real solution requires a massive shift in how the international community values the lives of people in "fragile" states.