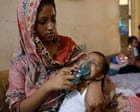
The death of over 100 children from measles in Bangladesh is not a failure of medical science; it is a failure of logistical execution and epidemiological surveillance. Measles maintains a basic reproduction number ($R_0$) between 12 and 18, making it one of the most contagious pathogens known to man. To achieve herd immunity and halt transmission, a population requires a minimum of 95% coverage with two doses of the measles-containing vaccine (MCV). When coverage dips below this threshold, the virus exploits "immunity gaps" with mathematical certainty. The current crisis suggests a systemic breach in the cold chain, a decline in routine immunization uptake, or a geographic concentration of susceptible individuals that has reached critical mass.
The Mechanistic Drivers of Measles Resurgence
Measles follows a predictable path of destruction when public health infrastructure degrades. The virus targets the respiratory tract, but its primary danger lies in its ability to induce "immune amnesia." It eliminates memory B and T cells, effectively resetting the immune system and leaving survivors vulnerable to secondary infections for months or years.
The Immunity Gap Equation
The susceptibility of a population is a function of:
- The Birth Rate: The constant influx of new, immunologically naive hosts.
- Vaccine Efficacy: Typically 93% for the first dose and 97% for the second.
- Coverage Rate: The percentage of the cohort successfully reached.
In Bangladesh, the mortality rate exceeding 100 individuals indicates that the outbreak has moved beyond isolated clusters into a generalized epidemic phase. This suggests that the "accumulation of susceptibles"—the number of children who missed their scheduled shots over several years—has surpassed the threshold required for sustained transmission.
The Triple Constraint of Outbreak Management
The Bangladesh measles vaccination drive is an emergency response to a breakdown in the following three operational pillars.
1. The Logistics of the Cold Chain
Measles vaccines are live-attenuated and highly sensitive to thermal fluctuations. They must be maintained between 2°C and 8°C. In rural or power-unstable regions of Bangladesh, any break in this temperature range renders the vaccine biologically inert. A drive that administers 10 million doses is meaningless if the "last mile" transport failed to maintain the cold chain. The high mortality rate may point to a false sense of security where children were "vaccinated" with degraded products, leading to primary vaccine failure.
2. Demographic Displacement and Density
Bangladesh’s high population density acts as a biological multiplier. In urban slums or refugee settlements, the $R_0$ of measles can exceed 20. When displacement occurs—whether due to climate events or economic migration—immunization records are lost, and follow-up for the second dose (MCV2) becomes nearly impossible. The current drive must account for "floating populations" that bypass standard district-level tracking systems.
3. The Surveillance-Response Lag
A death toll of 100 suggests that the virus was circulating undetected for weeks or months. Epidemiological surveillance in high-risk zones failed to trigger an "Early Warning and Response System" (EWARS) until the case fatality rate became impossible to ignore. This lag time allowed the virus to establish reservoirs in multiple districts, necessitates a much larger, more expensive "mop-up" campaign than would have been required if the index cases were contained.
Quantifying the Socio-Economic Cost of Delayed Intervention
The financial burden of a reactive vaccination drive is exponentially higher than routine immunization.
- Direct Costs: Procurement of millions of doses, cold-chain expansion, and hazard pay for healthcare workers.
- Indirect Costs: Diversion of healthcare resources from other critical areas like maternal health and nutrition, and the long-term economic loss of pediatric mortality.
- Opportunity Costs: The erosion of public trust. When a government launches a massive drive after 100 deaths, it signals a reactive rather than a proactive posture, which can fuel vaccine hesitancy.
Technical Barriers to Total Eradication
The deployment of a mass vaccination drive faces specific technical hurdles that go beyond simple supply.
The MCV1 vs. MCV2 Retention Gap
A single dose of the measles vaccine is insufficient for elimination. The second dose is critical for covering the 7% of children who do not develop immunity after the first. Bangladesh has historically struggled with "dropout rates," where children receive the first dose but do not return for the second. The current drive must prioritize the "zero-dose" children—those who have never entered the system—while simultaneously closing the gap for those who are partially immunized.
Diagnostic Deficits
In many rural clinics, measles is diagnosed clinically (by the presence of Koplik spots and a maculopapular rash). However, without laboratory confirmation (IgM antibody testing), it is difficult to distinguish measles from rubella or other febrile illnesses. This lack of granular data makes it difficult to map the exact genotype of the virus, which is necessary to track its origin and movement across borders.
Strategic Realignment of the Public Health Response
To move beyond the current crisis and prevent the next cycle of mortality, the intervention must shift from a "campaign" mindset to a "systemic" mindset.
Implementation of Digital Immunization Registries
The reliance on paper-based cards is a primary point of failure. A decentralized, digital registry linked to a national ID or birth registration system would allow for real-time tracking of coverage. This would enable health officials to identify specific villages or neighborhoods where coverage has dropped below the 95% threshold before an outbreak occurs.
Integration with Nutritional Support
Measles mortality is highly correlated with Vitamin A deficiency. The virus depletes Vitamin A stores, leading to blindness and increased severity of the disease. The vaccination drive should not be a standalone event; it must be bundled with high-dose Vitamin A supplementation. This is a physiological necessity to reduce the case fatality rate among those already infected or in the incubation period.
Hardening the Cold Chain with Solar-Direct Drive (SDD)
To eliminate the risk of thermal degradation, the infrastructure must transition to SDD refrigeration. This removes the dependency on a failing power grid or expensive diesel generators, ensuring that every dose administered is biologically active.
The 100 deaths reported are a lagging indicator of a system that was compromised years ago. The current mass vaccination drive is a necessary tactical maneuver, but it is not a strategy. True containment requires the aggressive closing of the MCV2 gap and the deployment of real-time, laboratory-backed surveillance. Failure to stabilize these underlying structural variables will result in a predictable recurrence of this crisis within the next three-to-five-year birth cohort cycle. The focus must shift from the number of doses delivered to the percentage of the population that remains immunologically protected over time.