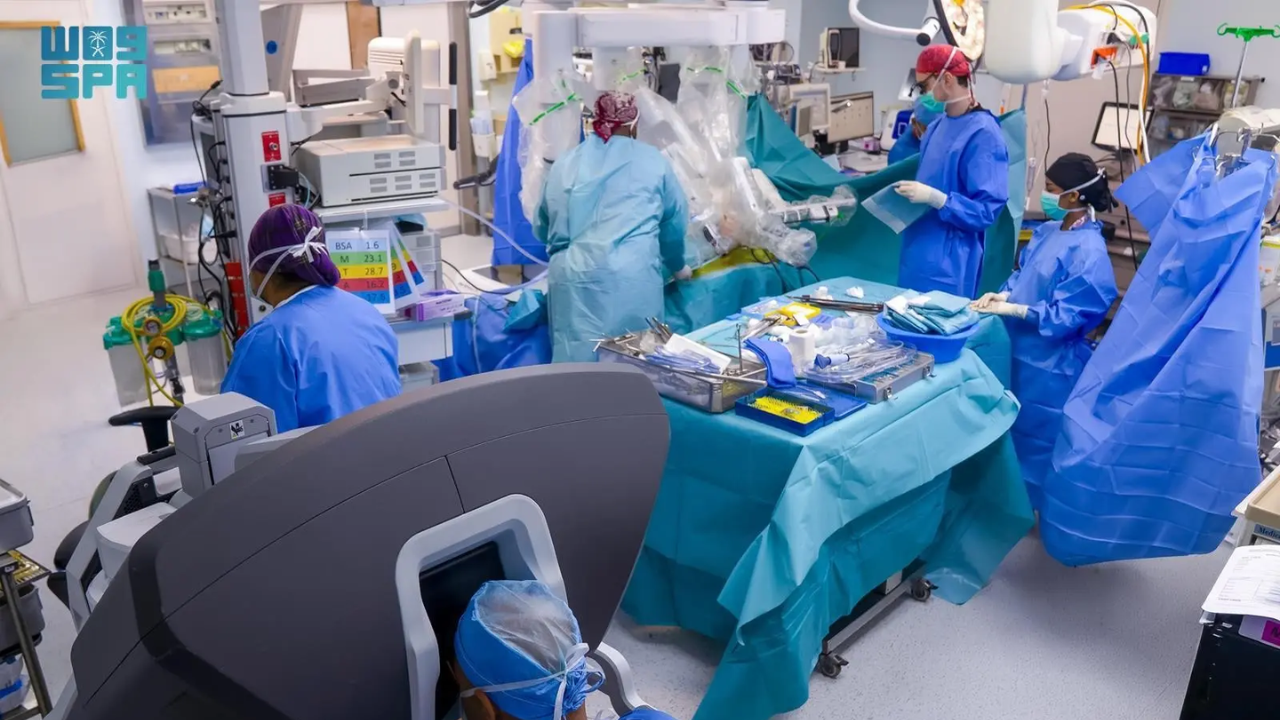
A surgical team in Jeddah recently achieved what many clinical centers only theorize about by successfully utilizing advanced robotic systems to treat Hirschsprung’s disease in children. This isn't just a win for a single hospital. It marks a fundamental shift in how the Gulf region handles complex congenital conditions that previously required invasive, high-risk open surgeries. By replacing the steady but limited human hand with high-definition, multi-jointed robotic arms, surgeons are now correcting bowel deformities through incisions measured in millimeters.
Hirschsprung’s disease is a grueling condition. It occurs when nerve cells are missing from parts of the large intestine, preventing the natural movement of waste. For an infant, this means chronic obstruction, severe infections, and a life tied to medical intervention. Traditional "pull-through" procedures involve significant trauma to the abdominal wall or the pelvic floor. The robotic approach, specifically the one pioneered at the King Faisal Specialist Hospital and Research Centre, bypasses the physical limitations of conventional laparoscopy.
The Mechanical Advantage Over Human Hands
Surgeons are limited by their physiology. Even the most elite paediatric surgeon has a tremor. It is tiny, nearly imperceptible, but it exists. Robotics eliminate that. The system used in these Hirschsprung’s cases filters out involuntary hand movements, providing a level of stability that is physically impossible for a human to maintain during a four-hour operation.
Furthermore, the robotic platform offers seven degrees of freedom. A human wrist cannot rotate 360 degrees while holding a needle. These instruments can. This dexterity is critical when working in the narrow, cramped pelvic cavity of a small child. When dealing with Hirschsprung’s, the surgeon must precisely dissect the diseased section of the colon and pull the healthy, nerve-rich segment down to the anus. One millimeter of error can lead to lifelong incontinence or nerve damage.
The Visualization Gap
Conventional surgery relies on the surgeon’s eyes or a 2D camera feed. Robotic systems provide a 10x magnified, 3D high-definition view. The surgeon sits at a console, immersed in the surgical field. They aren't looking at a screen across the room; they are "inside" the patient. This depth perception allows for the identification of tiny blood vessels and nerves that are easily overlooked in traditional open surgery.
Why Jeddah is Moving Faster Than the West
There is a common misconception that the most radical surgical advancements always originate in North America or Western Europe. This is no longer the case. The Gulf states, particularly Saudi Arabia, have invested billions into medical infrastructure that intentionally skips older generations of technology. While many Western hospitals are still debating the cost-benefit analysis of upgrading their robotic suites, Jeddah has integrated them into standard paediatric protocols.
This is a strategic play. By focusing on pediatric robotics, they are addressing a regional need for high-birth-rate populations where congenital anomalies like Hirschsprung’s appear more frequently due to genetic factors or late-stage screenings. The hospital in Jeddah isn't just buying machines; they are building a repository of data on robotic pediatric outcomes that will likely define global standards for the next decade.
The Real Cost of Innovation
Robotic surgery is expensive. A single system can cost upwards of $2 million, with thousands more in maintenance and disposable instrument costs per case. Critics often argue that these funds could be better spent on basic healthcare or preventative measures. However, this is a short-sighted perspective when looking at long-term patient recovery.
The "hospital stay" factor is the most compelling argument for the robot. Children undergoing traditional Hirschsprung’s repair often face weeks of recovery, pain management, and potential wound infections. Robotic cases consistently show faster bowel function return and significantly shorter hospital stays. If a child goes home three days earlier, the bed is freed for another patient, and the psychological trauma on the family is halved. The economic math shifts from the cost of the machine to the cost of the recovery cycle.
Training the Next Generation of Surgeons
We are witnessing the birth of the "digital native" surgeon. These practitioners are being trained on simulators before they ever touch a patient. At the Jeddah facility, the transition from console simulation to live surgery is a rigorous pathway. It requires a different type of hand-eye coordination than traditional surgery. It is a shift from manual labor to high-precision engineering.
The surgeon is no longer just a cutter. They are a systems operator. They must understand the physics of the robotic arms, the lag times of the software, and the spatial requirements of the internal instruments. This requires a level of technical literacy that traditional medical schools are only beginning to incorporate into their curricula.
The Complication of Complexity
Robotics are not a magic bullet. If a system fails mid-surgery—a rare but catastrophic event—the team must be prepared to convert to an open procedure instantly. This means every robotic surgeon must also be a master of the old-school techniques. There is a fear among industry veterans that the reliance on automation will erode these foundational skills.
In Hirschsprung’s surgery, the stakes are exceptionally high because the patient is growing. A robotic suture placed today must withstand the growth and physical changes of the child for the next eighty years. The data on long-term outcomes for pediatric robotic surgery is still being collected. We know the immediate results are superior, but we won't truly know the success of these Jeddah procedures until these children reach adulthood.
Beyond the colon
The success of the Hirschsprung’s initiative is a proof of concept. If you can perform a complex pull-through procedure on a child’s colon using a robot, you can apply those same principles to thoracic surgery, cardiac repairs, and tumor resections in pediatric oncology. The Jeddah team is effectively using Hirschsprung’s as a stress test for the entire robotic ecosystem.
The future of pediatric medicine isn't just "smaller tools." It is "smarter tools." We are approaching an era where the robot might provide real-time haptic feedback, telling the surgeon exactly how much pressure is being applied to a delicate tissue wall. This feedback loop will likely include AI-driven overlays that highlight "no-cut" zones in real-time based on the individual patient's pre-operative MRI scans.
The Global Pivot
Medical professionals from around the world are now looking toward the Middle East for this specific data set. The sheer volume of cases being handled in centers like King Faisal Specialist Hospital provides a statistical significance that smaller European centers struggle to match. This shift in the center of gravity for medical innovation is permanent.
The robotic revolution in Jeddah is a stark reminder that technology waits for no one. Hospitals that refuse to adapt or those that get bogged down in bureaucratic hesitation will find themselves obsolete. The children being treated today in Saudi Arabia are receiving a standard of care that was considered science fiction twenty years ago. The question is no longer whether robots should be in the operating room, but how quickly we can train enough surgeons to sit at the console.
Surgery is evolving from a craft of intuition into a science of precision. The move away from the "big incision" philosophy is a victory for the patient. It minimizes pain, reduces scarring, and gets children back into their homes faster. While the initial headlines focused on the "history-making" nature of the Jeddah surgery, the real story is the silent, efficient, and relentless precision of the machine that is now a permanent fixture in the pediatric ward.
The scalpel is being retired. The joystick is taking its place.